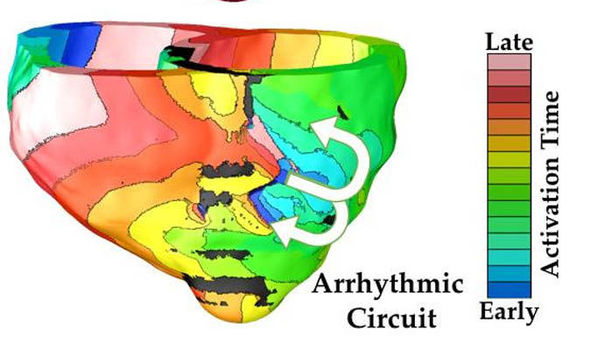
Personalised 3D computer models of patients’ hearts have been created to help cardiologists carry out life saving treatments.
The virtual organs, for instance, can work out a heart attack victims’ risk of developing a potentially fatal irregular beat.
They can then be surgically implanted with a defibrillator, a device that applies electric shocks to the heart when its rhythm goes out of kilter.
Arrhythmias or heart rhythm problems are experienced by more than two million people a year in the UK.
Sudden death due to arrhythmia is a leading cause of death in the industrialised world and kills 100,000 Britons every year.
Some of these could be avoided if the arrhythmias were diagnosed earlier.
But identifying the most vulnerable is difficult, because of the differences in the geometry of individual hearts, meaning defibrillators are limited in their therapeutic efficiency.
Many people are needlessly put through the invasive procedure and exposed to the possible complications that come with it.
Currently, cardiologists make their decision based on the patient’s ejection fraction – the proportion of blood that is pumped out of the heart with every beat.
If this number is below 35 per cent, then doctors advise the patient to have the implant.
Lots of patients are getting implants based on this strategy.
But in the first year afterwards, just five per cent will go on to develop arrhythmias and receive a necessary shock.
In other words, twenty devices are implanted for every one life saved.
So Professor Natalia Trayanova and colleagues used MRI (magnetic resonance imaging) scans to make detailed computer models of the electrical activity and shape of the hearts of 41 individual patients who had experienced a heart attack.
Combining computations of the geometry of the organ’s muscular wall and the degree of electrical instability in the heart enabled the researchers to assess the likelihood of each ‘virtual heart’ to develop an irregular heart beat.
They tested their results retrospectively using available clinical data from the patients, and found their approach was much more successful at predicting future life threatening changes in heart rhythm than current clinical methods.
Professor Natalia Trayanova, of Johns Hopkins University, Baltimore, said: “The approach could eliminate many unnecessary defibrillator implantations and their associated complications – infections, device malfunctions and inappropriate shocks – benefiting innumerable patients.”
Although not yet validated in an independent cohort of patients, the researchers believe the non invasive, personalised risk assessment tool has the potential to prevent sudden death from arrhythmia and eliminate many unnecessary implantations of defibrillators.
Prof Trayanova said: “This is the first study to develop a significant number of patient derived computational models of the heart and apply them to address a clinical need.
“Previous cardiac electrophysiological models have been limited to very small sample sizes or simplified geometries, and had been used to examine arrhythmia mechanisms.
“This study makes a leap forward in integrating image based computational modelling of the heart into heart disease diagnosis and treatment.
She works in the brand new field of computational medicine and added: “We believe computer modelling is poised to transform areas of medicine and serve as a vehicle to advance personalised approaches to human health.”
Her ‘heart’ is the most complete replica to date, mimicking the workings at the molecular scale, through the cellular scale, and up to the level of the whole organ, where muscle tissue expands and contracts with every heartbeat.
Starting with the patient’s MRI scans, specialists in computational cardiology can create a personalised model of the patient’s heart to study his or her unique ailment.
Doctors can then poke and prod the computerised organ in ways that simply are not possible with the real thing.
With these models at their disposal, cardiologists should be able to improve therapies, minimise the invasiveness of diagnostic procedures, and reduce health-care costs.
Prof Trayanova believes one day all patients with heart conditions, from babies to octogenarians, will have their virtual hearts tucked into their electronic medical records, which doctors can then use to plan their treatments, saying simulated hearts will be “able to prevent some real human hearts from breaking.”
The study is published in Nature Communications.